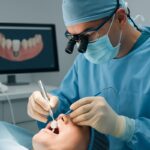
Gum disease in Bloomfield Hills, MI, also known as periodontal disease, is a common but preventable condition affecting the tissues surrounding teeth. Gum disease begins as gingivitis, characterized by red, swollen gums that may bleed easily during brushing or flossing. If left untreated, gum disease can progress to periodontitis, a more severe form of gum disease. Gum disease can lead to gum recession, bone loss, and ultimately, tooth loss.
Moreover, research suggests a connection between gum disease and systemic health concerns. Continue reading to learn in more detail how untreated gum disease can cause systemic health concerns.
How Does Gum Disease In Bloomfield Hills, MI Cause Systemic Health Concerns?
When gum disease progresses to its more severe form—periodontitis, bacteria can gain access to the bloodstream via the gum tissue. These bacteria then spread throughout the body and can potentially worsen existing health issues or even contribute to the development of new ones. A growing body of scientific evidence links untreated gum disease to a variety of systemic health concerns. The following are the specific systemic health concerns gum disease causes:
Cardiovascular Disease:
People with gum disease are nearly twice as likely to suffer from coronary artery disease compared to those without. The bacteria from inflamed gums can enter the bloodstream and attach to blood vessels, contributing to the formation of clots. These clots decrease blood flow to the heart, causing an elevation in blood pressure and increasing the risk of heart attacks.
Additionally, the body’s response to these trapped bacteria can cause inflammation leading to atherosclerosis—a condition that hardens the arteries and enhances the risk of heart disease. Therefore, maintaining good periodontal health can help manage cardiovascular disease.
Diabetes:
Gum disease can have a two-way relationship with diabetes. On the one hand, diabetes increases the body’s susceptibility to infections, including gum infections, making diabetics more prone to developing gum disease. On the other hand, severe gum disease can affect blood glucose control, potentially contributing to the progression of diabetes.
In patients with uncontrolled diabetes, increased levels of glucose in mouth fluids may help harmful bacteria flourish, leading to gum disease. Furthermore, individuals with diabetes often have a decreased ability to fight bacteria that invade the gums, further predisposing them to periodontal disease. This interaction makes maintaining good oral hygiene and regular dental check-ups crucial for people with diabetes.
What’s more, infections like periodontitis can increase insulin resistance and cause blood sugar levels to rise, making diabetes harder to control. The inflammation caused by gum disease can stimulate a rise in blood sugar, leading to diabetic complications. Therefore, appropriate periodontal care can also aid in the management and control of diabetes.
Rheumatoid Arthritis:
There’s a noteworthy link between gum disease and rheumatoid arthritis, an autoimmune disease that causes inflammation to the joints. Both diseases share a common denominator – inflammation. In gum disease, the inflammation arises due to the reaction of the body to the bacteria prevalent in plaque buildup. Similarly, rheumatoid arthritis is marked by chronic inflammation of the joints.
Specifically, the bacteria that cause periodontitis can increase inflammation throughout the body, including in the joints, making existing rheumatoid arthritis worse. Recent studies suggest that individuals with gum disease are more likely to have rheumatoid arthritis, underlining the importance of maintaining oral health to prevent or manage rheumatoid arthritis.
Cancer:
Intriguingly, recent research suggests a link between gum disease and certain types of cancer. The bacteria causing periodontitis can enter the bloodstream and reach different parts of the body. Once there, they can potentially stimulate a chronic inflammatory response, which is known to play a significant role in the development of cancer.
Studies have found that individuals with gum disease are at an elevated risk of developing cancers, such as pancreatic and kidney cancer.
Strokes:
Research indicates a connection between gum disease and the risk of having a stroke. The link lies in the bacteria causing periodontitis, which can enter the bloodstream through the inflamed gum tissue. Once the bacteria are in the bloodstream, they can travel to the brain and contribute to the formation of blood clots. The formation of these clots can interrupt the blood supply to the brain, leading to a stroke.
Moreover, the inflammation caused by gum disease can also lead to the damage of blood vessels, including those in the brain. Over time, this can narrow or block the blood vessels, thereby increasing the stroke risk. Thus, maintaining good oral health by preventing or treating gum disease can be a valuable strategy in reducing the risk of strokes.
In order to prevent these systemic health concerns from developing or worsening, it is important for people to maintain good oral health. Maintaining good oral health will not only preserve people’s teeth, it is a preventative measure against serious diseases, like cancer.
Explore Your Gum Disease Procedure Options With Dr. Lauren Anderson
If You have gum disease, then you should come to our quality office to receive gum disease procedures. With gum disease procedures, you will be able to treat or prevent systemic health concerns from developing.
Why wait to improve your smile and your overall health? Get in contact with Dr. Lauren Anderson and our exceptional team at our Anderson Periodontal Wellness office to schedule an appointment today!