
Join Dr. Anderson for a Lecture on 3 New Game Changers in Periodontal Field
Join Dr. Lauren Anderson on Monday, May 16 for an enlightening lecture on 3 new

Join Dr. Lauren Anderson on Monday, May 16 for an enlightening lecture on 3 new
Bloomfield Hills, Michigan Periodontist Dr. Lauren Anderson was recently featured on CBS where she shared her

Can My Oral Health Really Affect My Systemic Health? Yes! The most recent review article published
Above two patients presenting to Dr. Anderson’s office for the initial implant disease evaluation. On the
How Much Do You Know About Your Gum Health? Today periodontal disease affects over 64 million

Medications can cause problems in your mouth that may affect the gingiva (gums) and underlying structures
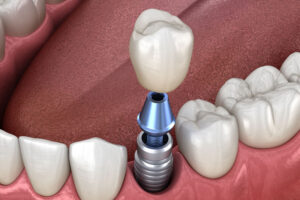
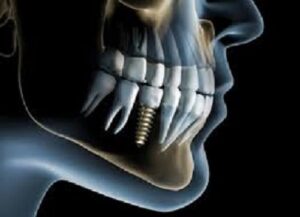
Dental implants are permanent tooth replacement options for patients missing one, some or all of their

Did you know periodontal disease is linked with many chronic diseases including diabetes mellitus, hypertension, athero-sclerotic

Above are two distinctly different photos. The picture to the left shows a 49 year old
