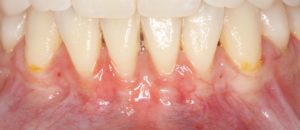
Mucogingival Defects, What Are They?
Mucogingival defects involve locations where gum is not attached to the tooth but rather mucosa or

Mucogingival defects involve locations where gum is not attached to the tooth but rather mucosa or

Did you know that keeping your smile healthy plays a big role in your overall health?
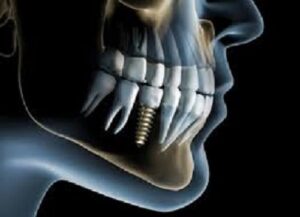
Above two patients presenting to Dr. Anderson’s office for the initial implant disease evaluation. On the

Medications can cause problems in your mouth that may affect the gingiva (gums) and underlying structures
