
Unveiling the Innovation Behind Dental Implants in West Bloomfield, MI
Dental implants have emerged as a pivotal advancement in modern dentistry, offering a permanent solution for

Dental implants have emerged as a pivotal advancement in modern dentistry, offering a permanent solution for
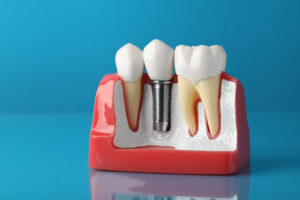
Preserving natural teeth remains a primary goal for a caring and dedicated periodontist, but sometimes teeth
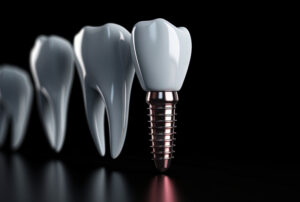
Having one or more missing teeth can prevent people from living their life normally. Luckily, even
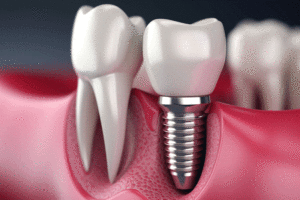
When people with missing teeth go to a quality and caring periodontist’s practice, they will be

When people have a full arch of missing teeth, they will want to get those teeth

Because everyone’s smile is unique, the cost of dental implant procedures will vary from patient to

Living without a complete arch of teeth negatively affects people’s quality of life. When people have
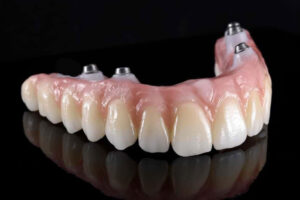
When people have tooth extractions, the area of the jawbone where their tooth has been extracted
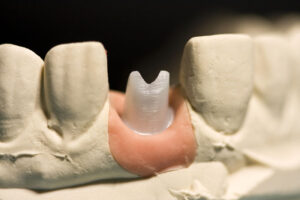
Interested in replacing failing or missing teeth with metal-free dental implants? Zirconia dental implants are a
